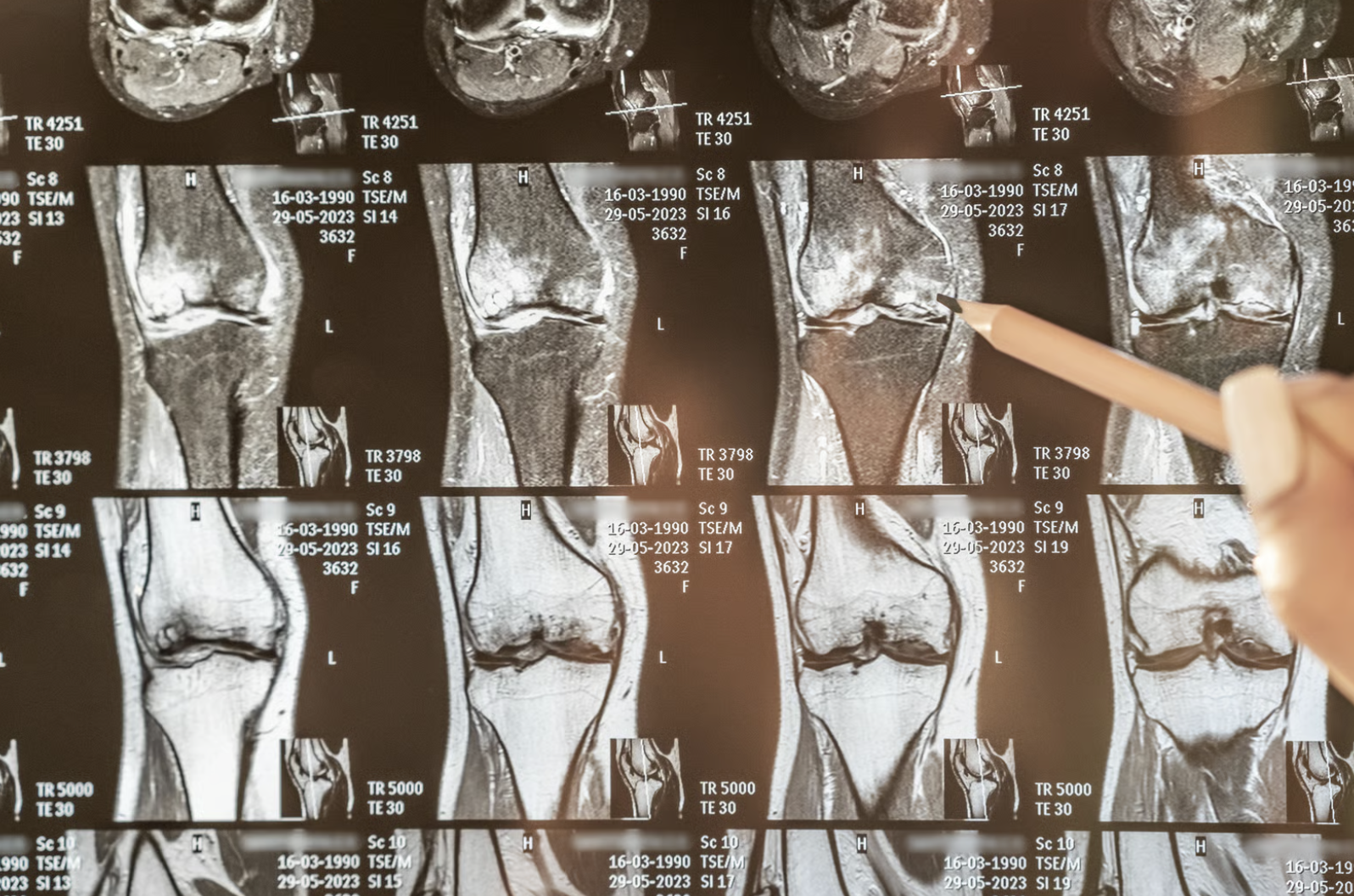
Knee osteoarthritis is a degenerative joint condition where the cartilage in the knee gradually wears down, leading to pain, stiffness, and reduced mobility. It develops in stages, each with specific symptoms and treatment needs. Recognising these stages can help determine when partial knee replacement may be an appropriate option to manage pain and preserve mobility.
Early Stage Knee Osteoarthritis (Stage 1)
In the early stage, the cartilage begins to show mild wear, but the joint still functions normally. Most people do not experience symptoms at this point.
Minimal cartilage damage: Small areas of softening occur on the cartilage surface, though the joint space appears normal on X-rays
Absent or mild symptoms: Most people experience no pain or stiffness, with occasional minor discomfort after prolonged activity
Normal joint function: Daily activities continue without limitation, and the knee maintains a full range of motion
Management approach: Treatment focuses on maintaining joint health through regular exercise and weight management
Mild Knee Osteoarthritis (Stage 2)
Cartilage breakdown becomes more apparent, though significant portions remain healthy. You may notice your first consistent symptoms during this stage.
Visible cartilage thinning: X-rays show slight joint space narrowing, and small bone spurs may develop around the joint edges
Morning stiffness: Joints feel stiff for 15-30 minutes after waking, improving with gentle movement throughout the day
Activity-related discomfort: Pain appears after extended walking, climbing stairs, or kneeling, but typically resolves with rest
Early intervention benefits: Physical therapy, anti-inflammatory medications, and joint injections can help slow progression
Moderate Knee Osteoarthritis (Stage 3)
At this stage, cartilage loss is more advanced, and symptoms begin to interfere with daily function. Many patients seek orthopaedic specialist evaluation to explore long-term treatment options.
Significant cartilage loss: Joint space narrowing becomes obvious on imaging, with larger bone spurs and possible loose cartilage fragments
Persistent pain patterns: Discomfort occurs during normal walking, with pain lasting several hours after activity
Movement limitations: Climbing stairs becomes difficult, and you may notice reduced knee flexibility or occasional swelling
Treatment escalation: More structured management may include stronger medications, targeted physiotherapy, and evaluation for surgical options.
Severe Knee Osteoarthritis (Stage 4)
The cartilage has worn away substantially, leaving bone rubbing against bone in affected compartments. Symptoms significantly impact daily life and mobility.
Advanced joint destruction: Cartilage has largely disappeared from one or more knee compartments, with visible bone changes and large spurs
Constant discomfort: Pain persists even during rest, often disrupting sleep and requiring regular pain medication
Functional impairment: Walking becomes laboured, stairs feel impossible, and simple tasks like getting up from chairs cause distress
Surgical consideration: Partial or total knee replacement becomes the primary treatment option when conservative measures no longer provide relief
When Partial Knee Replacement Is Considered
Partial knee replacement suits patients whose arthritis affects only one compartment of the knee joint. This procedure preserves healthy cartilage and ligaments while replacing the damaged area.
Compartmental damage: Arthritis affects either the inner (medial), outer (lateral), or kneecap (patellofemoral) compartment, while others remain healthy
Intact ligaments: The anterior cruciate ligament (ACL) and other supporting structures function normally
Suitable anatomy: Your knee shape and alignment allow for partial replacement components to fit properly
Realistic expectations: You understand that partial replacement addresses specific compartmental arthritis rather than whole-joint problems
When to See an Orthopaedic Specialist
You should consult an orthopaedic specialist if knee pain persists despite rest, physiotherapy, or medications, or if it interferes with walking, climbing stairs, or daily activities. Other signs that warrant evaluation include swelling, joint stiffness, instability, or mechanical symptoms such as locking or clicking. Early assessment allows for accurate diagnosis and timely treatment planning, including surgical options when appropriate.
Conclusion
Understanding the stage of your knee osteoarthritis can help guide appropriate treatment decisions. For patients with isolated joint damage, partial knee replacement may offer pain relief while preserving healthy joint structures.
If your symptoms are worsening or current treatments are no longer effective, schedule a consultation with our Orthopaedic Hip & Knee Surgeon to explore your options and develop a personalised management plan.