Do you hear a popping sound when your knee locks during movement? The meniscus functions as your knee’s shock absorber – two C-shaped pieces of cartilage that cushion the space between your thighbone and shinbone. When torn, this structure can cause pain, swelling, and mechanical symptoms that significantly impact daily activities. Meniscus tears can occur from acute twisting injuries during sports or from gradual degeneration over time. Treatment approaches range from conservative management with physiotherapy to surgical intervention, depending on tear location, pattern, and patient factors.
Types of Meniscus Tears
Meniscus tears present in distinct patterns that influence treatment decisions. Radial tears cut across the meniscus fibres perpendicular to its C-shape, often occurring in the middle portion where the blood supply remains limited. These tears rarely heal without intervention due to poor vascularity in the affected zone.
Horizontal tears split the meniscus into upper and lower segments, creating a cleavage plane within the tissue. These degenerative tears may develop without significant trauma. The torn fragments can flip into the joint space, causing mechanical catching sensations.
Bucket-handle tears involve large portions of the meniscus displacing into the joint centre, frequently blocking full knee extension. Patients often experience sudden locking episodes in which the knee cannot fully straighten. This tear pattern typically requires surgical attention to restore knee motion.
Complex tears combine multiple tear patterns within the same meniscus, creating irregular tissue fragments. These tears often occur in degenerative menisci and present surgical challenges due to extensive tissue damage. Treatment decisions depend on fragment stability and remaining healthy tissue.
💡 Did You Know?
The outer third of the meniscus receives blood supply from surrounding capsular vessels, allowing tears in this “red zone” to heal naturally or after repair. The inner two-thirds lack blood vessels, making spontaneous healing unlikely in this “white zone.”
When Surgery Becomes Necessary
Persistent mechanical symptoms despite conservative treatment indicate surgical consideration. Locking episodes where the knee catches and cannot fully extend suggest displaced meniscal fragments requiring removal. Recurrent swelling after activities, particularly when accompanied by pain along the joint line, often reflects ongoing meniscal irritation.
Failed conservative management after 6-12 weeks warrants surgical evaluation. Physical therapy aims to strengthen surrounding muscles and improve knee mechanics, but cannot address structural meniscal damage. Patients experiencing ongoing pain, swelling, or instability despite dedicated rehabilitation may benefit from surgical intervention.
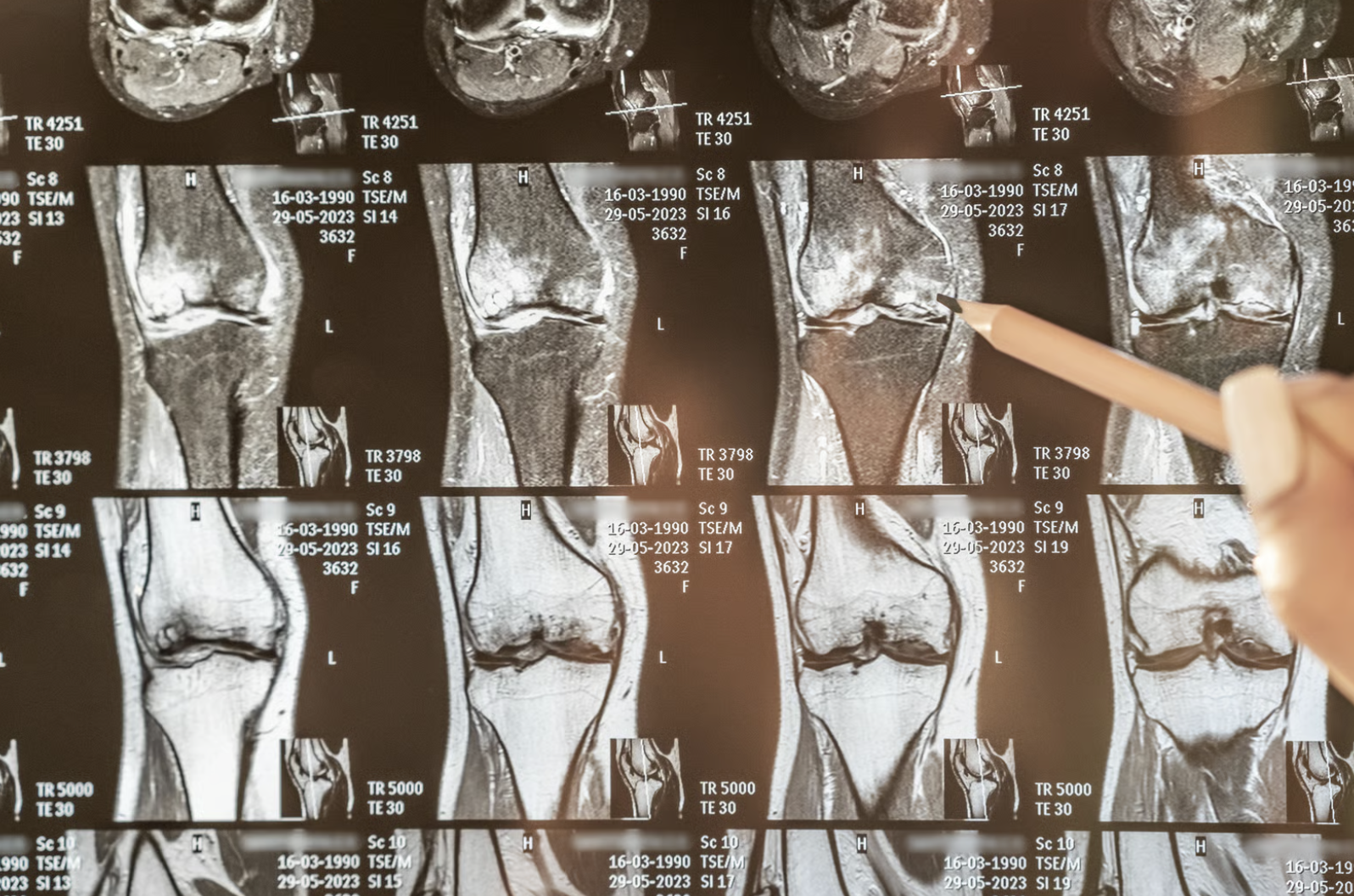
MRI findings guide surgical planning but must correlate with clinical symptoms. Imaging reveals tear location, pattern, and size while helping identify associated injuries. However, many individuals have asymptomatic meniscal changes on MRI, underscoring the need for clinical correlation in treatment decisions.
Age and activity level influence surgical timing and technique selection. Younger patients with acute tears in vascular zones often undergo repair procedures to preserve meniscal tissue. Older patients with degenerative tears may benefit from partial meniscectomy to address symptomatic fragments while preserving stable tissue.
Surgical Options
Arthroscopic Partial Meniscectomy
Arthroscopic partial meniscectomy removes unstable, torn fragments while preserving healthy meniscal tissue. Surgeons use specialised instruments through 2-3 small incisions to trim damaged portions, creating stable edges that won’t catch during knee motion. The procedure typically takes 20-40 minutes under regional or general anaesthesia.
Recovery is progressing, with patients walking immediately post-surgery and using crutches for comfort. Range-of-motion exercises begin within days, progressing to strengthening activities by weeks 2-3. Return to desk work occurs within 1-2 weeks, while physical jobs may require 4-6 weeks of recovery.
Meniscus Repair
Meniscus repair reattaches torn edges using sutures or devices, preserving the meniscus’s protective function. Suitable candidates have acute tears in the peripheral vascular zone, particularly younger patients with good healing potential. The procedure requires 30-60 minutes and uses arthroscopic or combined techniques depending on the tear location.
Post-repair protocols protect the healing tissue through controlled loading. Patients typically use crutches for 4-6 weeks, initially with restricted knee flexion. Physical therapy progresses gradually, emphasising range of motion before strengthening. Full recovery and return to sports requires 4-6 months for adequate tissue healing.
Meniscus Replacement
Meniscal allograft transplantation replaces severely damaged or absent meniscus tissue with donor grafts. This procedure suits younger patients with total meniscectomy who experience persistent pain and early arthritis. Surgeons size-match donor tissue and secure it using bone plugs or suture techniques.
Rehabilitation follows protocols over 6-9 months. The initial phases focus on graft protection and gradual range-of-motion restoration. Progressive weight-bearing begins around week 6-8, with strengthening activities introduced carefully. Return to impact activities may take 9-12 months following successful integration.
⚠️ Important Note
Smoking significantly impairs meniscal healing by reducing blood flow to repair sites. Patients undergoing meniscus repair may consult their healthcare professional regarding smoking cessation before surgery and throughout recovery to optimize healing potential.
Pre-Surgery Preparation
Medical clearance allows for safe surgery, particularly for patients with chronic conditions. Blood tests, ECG, and chest X-rays may be required based on age and medical history. Medication adjustments, especially for blood thinners and anti-inflammatory drugs, occur under physician guidance, typically 5-7 days pre-surgery.
Physical preparation may support surgical outcomes through “prehabilitation.” Strengthening exercises for the quadriceps and hamstrings may improve post-operative function. Range-of-motion exercises may help prevent stiffness, while cardiovascular conditioning may aid recovery. Ice application and elevation techniques learned pre-surgery may prove valuable post-operatively.
Home modifications can enhance comfort and safety during recovery. Installing grab bars in bathrooms, arranging ground-floor sleeping if needed, and preparing meals in advance may reduce post-surgical stress. Securing assistance for the first few days may help with proper rest and medication compliance.
Equipment preparation includes obtaining crutches, ice packs, and prescribed braces before surgery day. Loose-fitting clothing accommodates post-surgical swelling and dressings. Having entertainment and work materials within easy reach minimises unnecessary movement during initial recovery.
Recovery Timeline
Week 1-2: Initial Healing
Immediate post-operative care focuses on pain control and the reduction of swelling. Ice application for 20 minutes every 2-3 hours may help reduce inflammation. Elevation above heart level may enhance fluid drainage. Pain medications transition from stronger prescriptions to over-the-counter options as comfort improves.
Wound care maintains surgical site integrity. Keeping incisions clean and dry helps prevent infection, while waterproof dressings may allow showering after 48-72 hours. Observing for excessive drainage, worsening redness, or fever helps detect the problem early.
Early mobilisation may help prevent stiffness and promote circulation. Ankle pumps, quadriceps sets, and gentle knee bending within comfort limits may begin as advised by your orthopaedic surgeon. Weight-bearing status depends on the procedure type: partial meniscectomy patients often walk immediately, while repair patients may remain non-weight-bearing.
Week 3-6: Progressive Rehabilitation
Physical therapy may intensify with formal sessions as recommended by your orthopaedic surgeon. Range-of-motion goals may include achieving 90 degrees of flexion by week 3 and full extension throughout. Strengthening exercises may progress from isometric to resistive activities using bands and light weights.
Functional activities may gradually resume based on the surgical procedure and individual progress. Stationary cycling may typically begin when knee flexion reaches 100-110 degrees. Swimming and water walking may provide low-impact conditioning options. Daily activities like driving may resume when reaction times and comfort allow safe operation, as determined by your orthopaedic surgeon.
Week 7-12: Return to Activities
Advanced strengthening may target sport-specific movements and dynamic stability. Plyometric exercises, agility drills, and progressive running programs may help prepare athletes for return to play. Non-athletes may focus on recreational activities and occupational demands.
Ongoing assessment guides activity progression through objective testing. Single-leg hop tests, strength measurements, and functional questionnaires may track recovery milestones. A gradual return to complete activities may help prevent re-injury while building confidence in knee function.
✅ Quick Tip
Maintain a recovery journal documenting daily pain levels, swelling changes, and activity tolerance. This information may help your surgeon and physiotherapist adjust rehabilitation protocols based on your individual progress patterns.
Potential Complications
Infection remains rare but requires vigilance for early detection. Warning signs include:
- Increasing pain after initial improvement
- Wound drainage
- Fever above 38.5°C
- Expanding redness around incisions
Medical attention and antibiotics typically resolve superficial infections.
Blood clots pose risks that require preventive measures. Early mobilisation, ankle exercises, and compression stockings reduce clot formation. Calf pain, swelling, or breathing difficulties warrant medical evaluation to rule out deep vein thrombosis or pulmonary embolism.
Persistent stiffness occasionally develops despite appropriate therapy. Arthrofibrosis – excessive scar tissue formation – limits range of motion and may require manipulation under anaesthesia or arthroscopic release. Early motion and anti-inflammatory strategies minimise this risk.
Re-tear or repair failure occurs in some cases, particularly with complex tears or compromised healing environments. Gradual activity progression and compliance with post-operative restrictions reduce the risk of failure. Revision surgery options exist, but depend on the quality of the remaining meniscal tissue.
What Orthopaedic Surgeons Say
Clinical examination often provides valuable information in addition to MRI findings. Many patients present with meniscal tears on imaging that don’t correlate with their symptoms. Physical examination, identifying specific joint line tenderness, mechanical symptoms, and provocative test findings, guides treatment selection.
Tissue-preservation philosophy drives modern meniscal-surgery approaches. Removing meniscal tissue accelerates arthritis development, making repair attempts worthwhile when feasible. Even partial preservation through selective trimming maintains improved long-term joint health than complete removal.
Meniscus surgery addresses mechanical symptoms but cannot reverse existing arthritis or result in complete pain elimination. Goal-setting during consultation helps patients understand achievable outcomes based on their specific pathology.
Putting This Into Practice
- Schedule a consultation when conservative measures fail to resolve mechanical symptoms after dedicated trial periods. Document specific activities that trigger pain, catching sensations, or swelling episodes to help your surgeon understand your functional limitations. Bring previous imaging and treatment records to avoid redundant testing.
- Optimise your general health before surgery through smoking cessation, weight management, and diabetes control if applicable. These modifiable factors can impact surgical outcomes and healing potential. Begin pre-operative exercises as recommended by your healthcare team to support post-operative function.
- Arrange post-operative support systems, including transportation, home assistance, and work modifications. Clear your schedule for initial recovery phases and plan a gradual return to activities. Prepare questions about expected timelines specific to your tear pattern and planned procedure.
- Follow the full rehabilitation protocol as prescribed by your healthcare team, regardless of early symptom improvement. Premature return to activities risks re-injury and may affect long-term outcomes. Communicate openly with your surgical team about progress, setbacks, or concerns throughout recovery.
- Research your physiotherapy options and book initial appointments before surgery. Establishing care continuity can facilitate a smooth transition from surgical recovery to active rehabilitation. Select therapists with experience in post-meniscal surgery protocols for appropriate guidance.
When to Seek Professional Help
- Knee locking prevents full extension or flexion
- Recurrent swelling after routine daily activities
- Sharp catching sensations during weight-bearing movements
- Joint line pain persists despite rest and anti-inflammatory measures
- Feeling of knee instability or giving way during walking
- Night pain disrupting sleep patterns
- Lack of improvement after 6-12 weeks of conservative treatment
- Mechanical symptoms interfering with work or recreational activities
Commonly Asked Questions
How long before I can return to sports after meniscus surgery?
Return timelines vary significantly by procedure type. Partial meniscectomy patients often resume sports within 6-8 weeks following graduated rehabilitation. Meniscus repair requires 4-6 months for tissue healing before sport-specific training begins. Individual factors, including tear location, associated injuries, and sport demands, influence specific timelines.
Will I develop arthritis after meniscus surgery?
Meniscectomy increases the risk of arthritis in proportion to the amount of tissue removed, though progression varies from person to person. Preserving meniscal tissue through repair or limited trimming maintains improved joint mechanics. Post-surgical rehabilitation, emphasising strength and proper biomechanics, helps protect remaining cartilage from accelerated wear.
Can a torn meniscus heal without surgery?
Peripheral tears in the vascular zone occasionally heal with conservative treatment, including activity modification and physiotherapy. Most tears in the avascular central zone cannot heal independently due to the absence of a blood supply. Small, stable degenerative tears may become asymptomatic through rehabilitation despite persistent structural defects.
What’s the difference between meniscus repair and removal?
Repair procedures reattach torn edges with sutures to preserve meniscal function, resulting in a longer recovery but maintaining joint protection. Removal (partial meniscectomy) eliminates unstable fragments causing symptoms, allowing faster recovery but reducing long-term shock absorption. Treatment recommendations depend on tear characteristics and healing potential.
How successful is meniscus surgery?
Partial meniscectomy can eliminate mechanical symptoms when addressing appropriate pathology. Repair outcomes depend on tear location, with peripheral repairs healing well in young patients. Complex tears in degenerative menisci show lower success rates regardless of technique.
Next Steps
Arthroscopic techniques effectively address mechanical symptoms by preserving tissue when possible or selectively removing it when necessary. Successful outcomes depend on proper tear assessment and appropriate technique selection based on individual pathology and healing potential.
If you’re experiencing persistent knee locking, catching, or swelling that interferes with daily activities, schedule an evaluation with an orthopaedic surgeon.