Knee osteoarthritis occurs when the protective cartilage in the knee joint gradually wears down, leading to bone-on-bone contact. This progressive condition affects the entire joint, including bones, cartilage, ligaments, and muscles. As the joint deteriorates, individuals may experience pain, stiffness, and reduced mobility, making activities like walking, climbing stairs, or standing up more challenging.
This guide explores the symptoms, causes, diagnosis, and treatment options for knee osteoarthritis, providing insights into how to manage the condition effectively.
Recognising the Symptoms of Knee Osteoarthritis
Knee osteoarthritis develops gradually, with symptoms worsening over time. Common signs include:
Pain During Movement: Pain occurs during walking, climbing stairs, or other weight-bearing activities. It often worsens with prolonged use and improves with rest.
Morning Stiffness: The knee feels stiff after waking up or sitting for long periods. This usually resolves within 30 minutes of movement.
Reduced Range of Motion: The knee becomes less flexible, making it difficult to fully bend or straighten. This can affect daily tasks such as getting in and out of a car.
Joint Swelling: Swelling may occur, especially after physical activity or towards the end of the day, causing tightness and discomfort.
Clicking or Crunching Sounds: Movement may be accompanied by clicking or a grinding sensation due to rough cartilage surfaces rubbing against each other.
What Causes Knee Osteoarthritis?
Multiple factors contribute to the development and progression of knee osteoarthritis, affecting joint health over time. Common causes include:
Age: The risk increases with age due to natural joint wear. Most cases occur in people over 50.
Previous Knee Injuries: Past injuries, such as meniscus tears, ligament damage, or fractures, can lead to osteoarthritis later in life.
Excess Weight: Additional body weight places extra strain on the knee. Each extra kilogram adds roughly four times the force on the knee during walking.
Genetics: Some individuals inherit a predisposition to osteoarthritis. Genetic factors can affect cartilage structure and durability.
Occupational Factors: Jobs that involve frequent kneeling, squatting, or heavy lifting can increase joint stress and contribute to cartilage breakdown.
Types of Knee Osteoarthritis
Osteoarthritis affects different parts of the knee joint, leading to varied symptoms and progression patterns.
Medial Compartment Osteoarthritis
Affects the inner side of the knee. Since this area bears most of the body’s weight, wear can lead to a bow-legged appearance, increasing stress on the inner knee.
Lateral Compartment Osteoarthritis
Affects the outer side of the knee. It is less common but can develop due to injuries or anatomical factors, sometimes leading to a knock-kneed stance.
Patellofemoral Osteoarthritis
Occurs between the kneecap (patella) and thighbone (femur). It often causes discomfort during activities that involve bending the knee, such as climbing stairs or standing up from a seated position. In some cases, kneecap alignment issues contribute to worsening symptoms.
How Knee Osteoarthritis Is Diagnosed
Accurate diagnosis helps determine the severity of the condition and the most suitable treatment approach. Several methods are used to confirm osteoarthritis and assess joint damage.
Physical Examination: The doctor evaluates knee movement, stability, and alignment. This includes checking for swelling, tenderness, and crepitus (crackling sounds) while moving the joint. Walking patterns and muscle strength around the knee are also assessed.
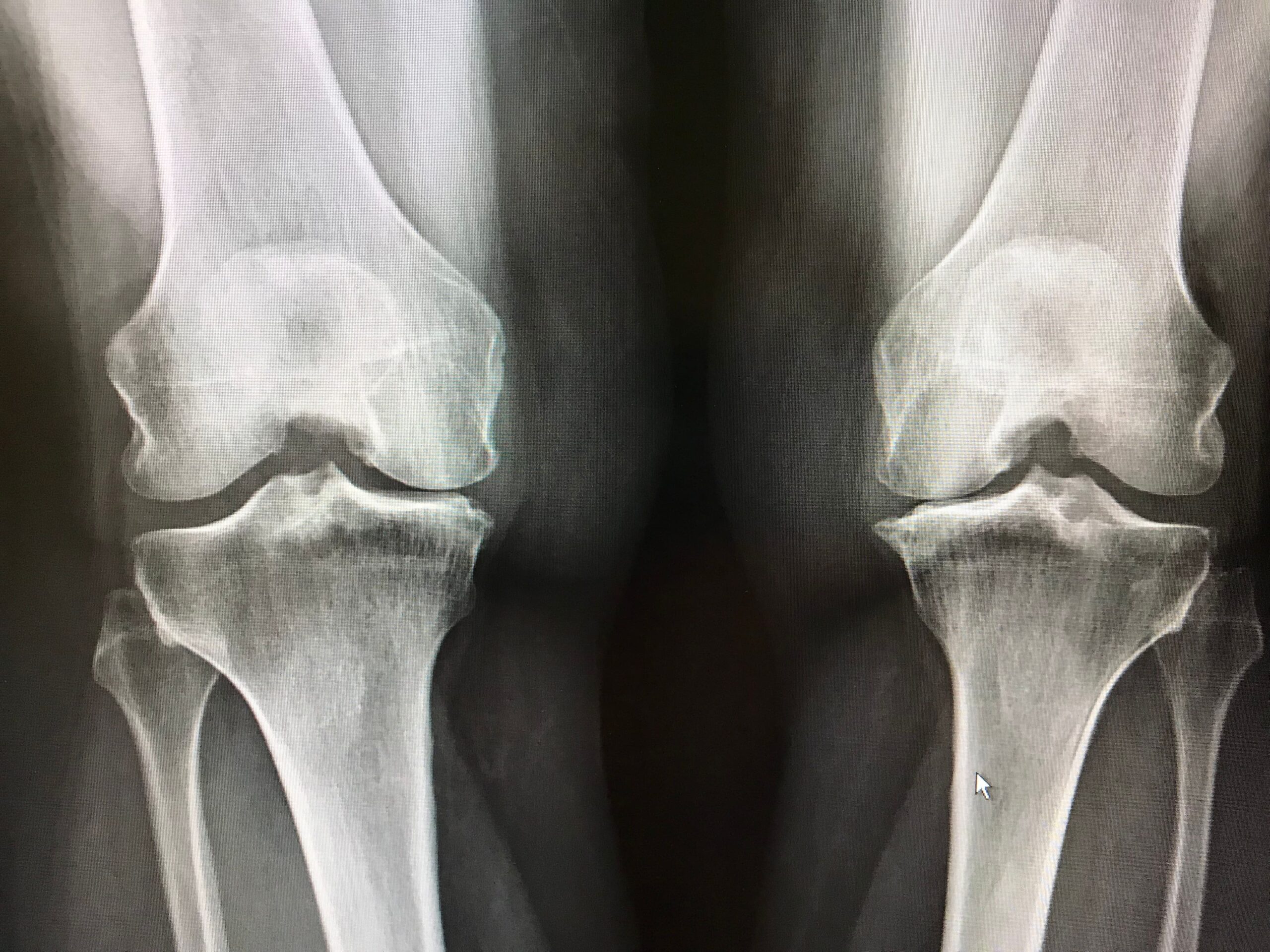
X-rays: Weight-bearing X-rays show joint space narrowing, bone spurs (osteophytes), and alignment changes. These images help track disease progression.
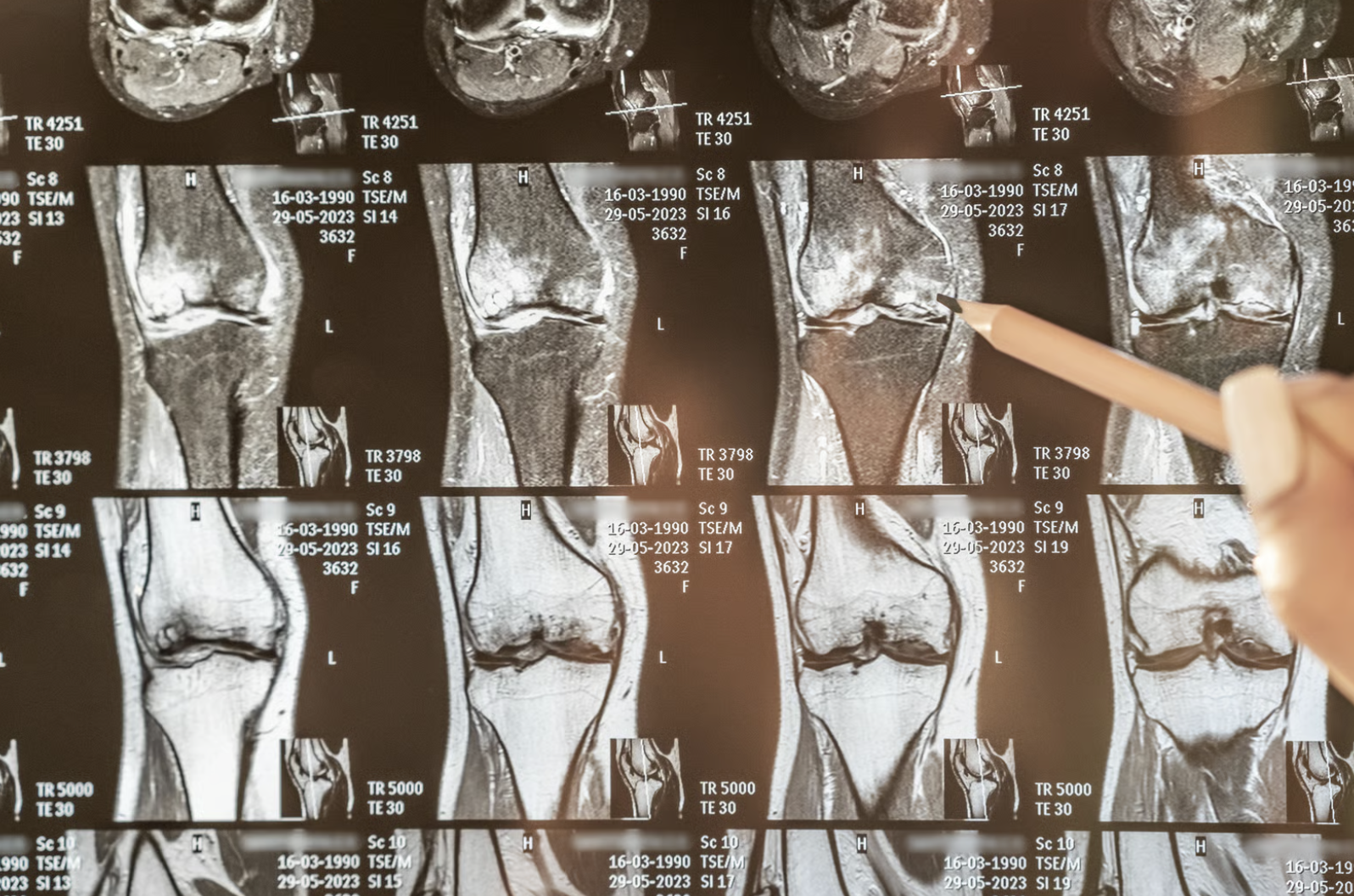
MRI Scanning: An MRI provides detailed images of soft tissues, including cartilage, menisci, and ligaments. It is useful for evaluating complex cases or planning surgery and can detect early cartilage changes that may not appear on X-rays.
Blood Tests: While osteoarthritis cannot be diagnosed through blood tests, these can help rule out other conditions like rheumatoid arthritis or gout by measuring inflammation markers.
Treatment Options for Knee Osteoarthritis
Management of knee osteoarthritis focuses on relieving symptoms, maintaining function, and slowing progression.
Non-Surgical Approaches
Exercise and Physical Therapy
Low-impact exercises strengthen the muscles around the knee and improve flexibility. A physiotherapist can tailor exercises to individual needs and guide proper movement to reduce joint strain.
Weight Management
Reducing excess weight helps decrease stress on the knee joint. A structured plan combining nutrition and exercise supports long-term joint health.
Medications
Non-steroidal anti-inflammatory drugs (NSAIDs) help manage pain and inflammation. Topical treatments, such as creams and gels, provide localised relief with fewer systemic side effects.
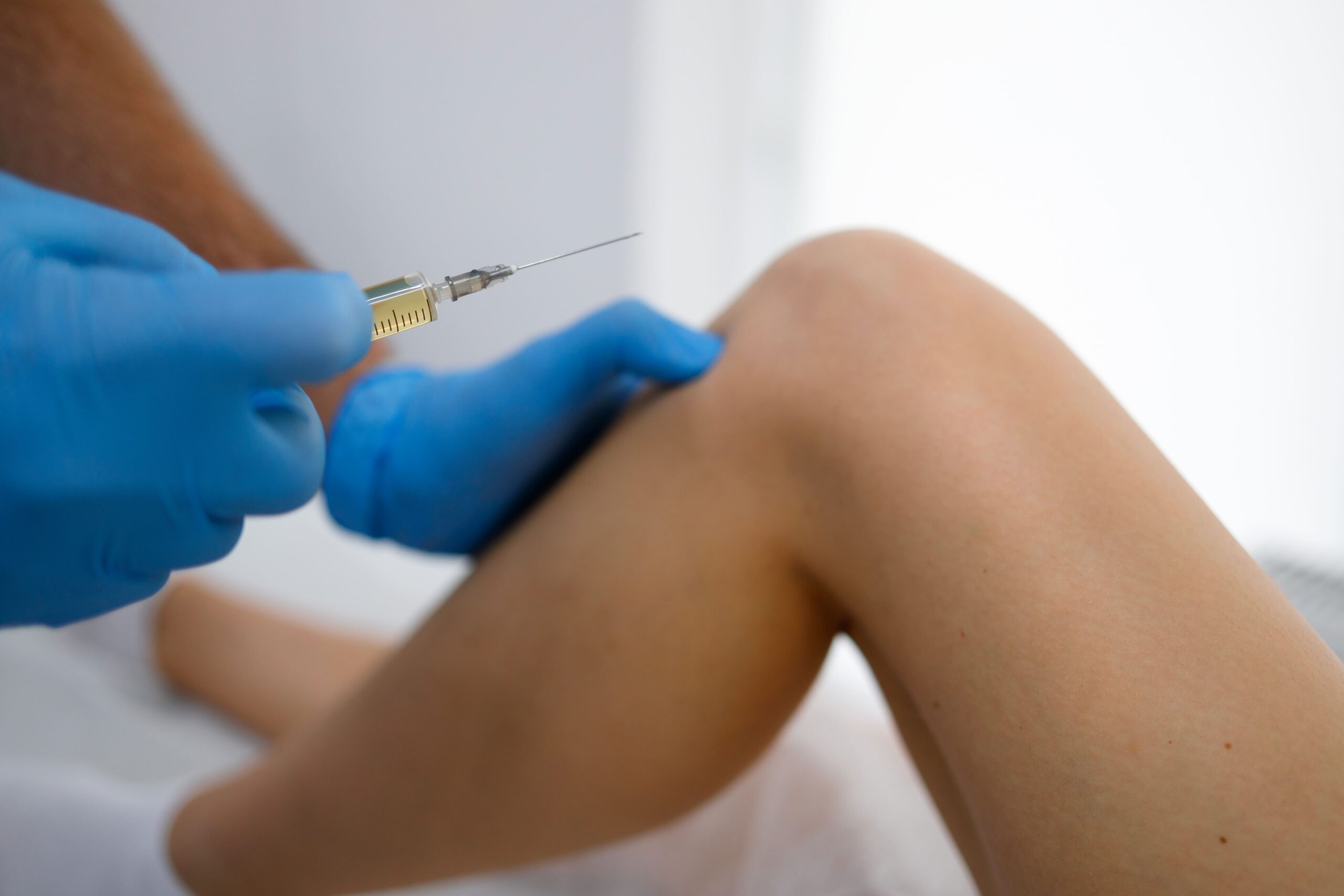
Injections: Corticosteroid injections help reduce inflammation and provide temporary pain relief. Hyaluronic acid injections supplement the joint’s natural lubrication, which may improve comfort for several months.
Surgical Treatment
Arthroscopy
A minimally invasive procedure in which a surgeon makes small incisions to insert a camera and specialised instruments into the knee joint. This allows for the removal of loose cartilage, smoothing of rough joint surfaces, and addressing minor structural issues. Arthroscopy is typically used for symptom relief in selected cases rather than as a long-term solution for advanced osteoarthritis.
Osteotomy
A surgical procedure that involves reshaping the tibia or femur to shift weight away from the damaged part of the knee joint. By redistributing stress to healthier areas, this approach can help relieve pain and delay the need for joint replacement, particularly in younger or more active patients.
Joint Replacement
When osteoarthritis has severely damaged the knee joint, a partial or total knee replacement may be recommended. This procedure involves removing worn-out joint surfaces and replacing them with artificial components designed to restore movement and reduce pain. Joint replacement is typically considered when other treatments no longer provide sufficient relief.
Managing Knee Osteoarthritis
Ongoing management helps maintain mobility and slow progression. Regular exercise, including low-impact activities such as swimming or cycling, keeps the knee flexible and strengthens surrounding muscles. Using proper techniques when moving or lifting can minimise unnecessary joint strain.
Supportive footwear improves stability, and assistive devices like braces or walking aids may reduce pressure on the knee. Maintaining a healthy weight further reduces excess stress on the joints, helping to manage symptoms more effectively.
Conclusion
Knee osteoarthritis is a progressive condition, but with the right approach, symptoms can be managed to maintain mobility and quality of life. Early intervention, lifestyle adjustments, and appropriate treatment can help slow progression and reduce discomfort.
If you are experiencing persistent knee pain or stiffness, schedule a consultation to explore your treatment options.