Can you imagine your knee pain completely disappearing after years of limitation? While conservative treatments like physiotherapy and medications help many patients, certain conditions require surgical intervention. Current orthopaedic procedures range from minimally invasive arthroscopy to total joint replacement, each designed for specific knee problems and patient needs.
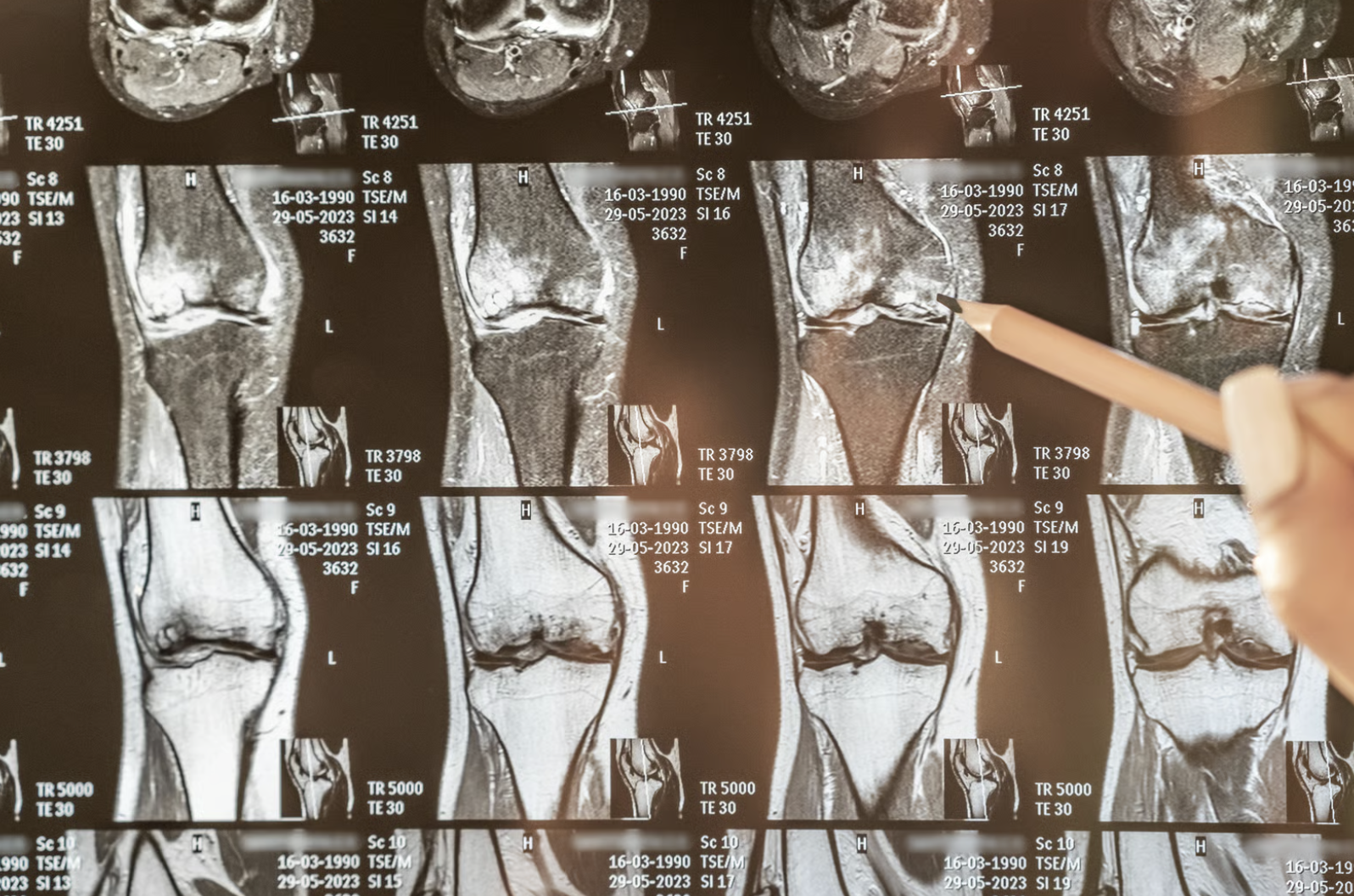
Your orthopaedic surgeon determines surgical candidacy based on several factors: severity of structural damage visible on MRI or X-ray, failure of conservative treatments over 3-6 months, impact on daily activities, and overall health status. Age alone rarely determines surgical suitability – functional limitations and pain levels guide treatment decisions.
Knee Arthroscopy
Arthroscopy uses a pencil-sized camera (arthroscope) inserted through small incisions to diagnose and treat knee problems. The surgeon views the joint interior on a monitor while using miniature instruments to repair damage.
Standard arthroscopic procedures include:
- Meniscus repair or removal: Torn meniscus fragments cause catching, locking, or persistent pain
- Cartilage debridement: Smoothing rough cartilage surfaces that cause inflammation
- Loose body removal: Extracting bone or cartilage fragments floating in the joint
- Synovectomy: Removing the inflamed joint lining in inflammatory arthritis
- Ligament reconstruction: ACL or PCL repair using grafts from tendons
The procedure typically takes 30-90 minutes under general or regional anaesthesia. Patients usually return home the same day. Recovery involves:
- Week 1-2: Crutches or walking aid, gentle range-of-motion exercises
- Week 3-4: Progressive weight-bearing, physiotherapy begins
- Week 6-8: Return to low-impact activities
- Months 3-6: Full recovery for complex repairs
Arthroscopy may be suitable for mechanical problems, such as meniscus tears or loose bodies. However, it provides limited benefit for advanced arthritis where cartilage loss is widespread.
Partial Knee Replacement (Unicompartmental)
Partial knee replacement replaces only the damaged compartment of the knee joint while preserving healthy bone and tissue. The knee has three compartments: medial (inside), lateral (outside), and patellofemoral (kneecap). When arthritis affects only one compartment, partial replacement offers targeted treatment.
Candidates may have:
- Isolated compartment arthritis confirmed by imaging
- Intact ACL and other ligaments
- Minimal deformity (less than 10 degrees)
- Good range of motion (at least 90 degrees flexion)
- Body weight appropriate for implant longevity
The surgery involves:
- Removing damaged cartilage and minimal bone from the affected compartment
- Implanting metal components in the femur and tibia
- Inserting a plastic spacer between metal surfaces
- Preserving all ligaments and unaffected compartments
Advantages compared to total replacement include:
- Smaller incision (7-10cm vs 15-20cm)
- Less bone removal preserves future options
- More natural knee movement and proprioception
- Recovery time may be shorter (discharge in 1-2 days)
- Lower complication risk
Recovery timeline:
- Day 1: Walking with physiotherapist assistance
- Week 2: Walking independently, climbing stairs
- Week 6: Driving, returning to desk work
- Month 3: Low-impact sports like swimming, cycling
- Month 6: Recovery
Partial replacements typically last 15-20 years. If the implant wears out or arthritis develops in other compartments, conversion to total replacement remains straightforward.
Total Knee Replacement
Total knee replacement removes all damaged cartilage and reshapes bone ends to accommodate prosthetic components. Current implants replicate natural knee geometry while providing smooth, pain-free movement.
The procedure involves:
- Removing damaged cartilage from the femur, tibia, and patella
- Reshaping bone ends using cutting guides
- Cementing metal components to the femur and tibia
- Inserting a plastic bearing surface between metal parts
- Resurfacing or replacing the kneecap if needed
Surgical approaches include:
- Traditional: 15-20cm incision, comprehensive joint exposure
- Minimally invasive: 10-12cm incision, less muscle disruption
- Computer-assisted: Navigation technology for alignment
- Robotic-assisted: Pre-operative CT planning with robotic execution
Material options:
- Standard cobalt-chromium: Durable, suitable for most patients
- Oxidised zirconium: Reduced nickel content for metal sensitivity
- Ceramic components: For younger patients or those with nickel allergy
- Rotating platform: Allows bearing rotation, reducing wear
Post-operative protocol:
- Day 0-1: Pain management, ankle pumps, assisted standing
- Day 2-3: Walking with a frame, knee bending exercises
- Week 1-2: Discharge home, outpatient physiotherapy begins
- Week 6: Walking without aids, 90-degree flexion goal
- Month 3: Return to normal activities, some sports
- Month 6-12: Maximum improvement achieved
Knee replacements have good longevity—most function well for many years. Factors affecting implant lifespan include patient weight, activity level, and implant positioning.
Osteotomy
Osteotomy realigns the leg by cutting and repositioning bone to shift weight from damaged to healthy cartilage. This procedure may be suitable for younger patients with isolated compartment arthritis and malalignment.
High tibial osteotomy (most common type) involves:
- Creating a wedge-shaped cut in the upper tibia
- Opening or closing the wedge to correct alignment
- Securing with plates and screws
- Allowing the bone to heal in a new position
Candidate criteria:
- Age typically under 60 with an active lifestyle
- Isolated medial compartment arthritis
- Varus (bow-legged) deformity less than 15 degrees
- Good range of motion
- Healthy lateral compartment and ligaments
Recovery requires patience:
- Week 0-6: Non-weight bearing with crutches
- Week 6-12: Progressive weight bearing
- Month 3-4: Full weight bearing, intensive physiotherapy
- Month 6: Return to impact activities
- Year 1: Bone fully consolidated
Osteotomy preserves the natural knee joint and permits high-impact activities after healing. Success depends on surgical planning and patient compliance with rehabilitation. The realignment may provide years of symptom relief before potential conversion to knee replacement.
Making Your Surgical Decision
Choosing knee surgery involves evaluating pain severity, functional limitations, imaging findings, and personal goals. Your orthopaedic surgeon will discuss:
- Conservative treatment adequacy: Have medications, injections, and physiotherapy been maximised?
- Timing considerations: Earlier intervention for mechanical problems, delayed for stable arthritis
- Activity expectations: Desired post-operative function guides procedure selection
- Medical fitness: Cardiac, respiratory, and metabolic health affect surgical safety
- Support system: Post-operative assistance impacts recovery success
💡 Did You Know?
Some knee replacement patients report forgetting which knee was operated on after full recovery, as current implants closely mimic natural joint movement and sensation.
What Our Orthopaedic Surgeon Says
Patient selection remains an important factor in surgical success. A meniscus tear in a 30-year-old athlete requires different treatment than the same tear in a 70-year-old with arthritis. We evaluate the whole patient – not just the MRI findings.
Knee surgery has evolved considerably. Today’s minimally invasive techniques, improved implants, and recovery protocols can help patients move with less pain. However, surgery represents one tool among many. We consider conservative options first and operate only when the benefits clearly outweigh the risks.
Putting This Into Practice
- Document your knee symptoms in a diary, including pain levels, triggering activities, and functional limitations, to share with your surgeon.
- Try conservative treatments thoroughly – at least 3 months of physiotherapy and activity modification before considering surgery.
- Prepare your home before surgery by installing grab bars, removing trip hazards, and setting up a recovery area on the ground floor.
- Arrange post-operative support from family or friends for the first two weeks when mobility is most limited.
- Research your surgeon’s qualifications for your procedure and ask about their approach and patient outcomes.
When to Seek Professional Help
- Knee pain persists beyond several weeks despite rest and medication
- Mechanical symptoms like locking, catching, or giving way
- Swelling that doesn’t resolve with elevation and ice
- Inability to fully straighten or bend the knee
- Night pain disrupts sleep regularly
- Difficulty with daily activities like climbing stairs or rising from chairs
- Previous injury with ongoing instability or discomfort
Commonly Asked Questions
How can I determine whether I need knee surgery?
Surgery becomes an option when conservative treatments fail to control pain or restore function after 3-6 months. Imaging demonstrating structural damage, combined with symptoms that limit daily activities, typically warrants surgical evaluation. Your orthopaedic surgeon assesses whether potential benefits outweigh surgical risks.
Which knee surgery lasts the longest?
Total knee replacements demonstrate a long track record, with modern implants functioning well for many years. Partial replacements also provide long-term results. Arthroscopy provides symptom relief for several years, depending on the progression of underlying arthritis. Osteotomy typically delays replacement for many years.
Can I return to sports after knee surgery?
Low-impact activities such as swimming, cycling, and golf are suitable after all knee surgeries, once the patient has healed. Arthroscopy patients often return to running and contact sports. Partial and total replacements allow recreational doubles tennis, hiking, and dancing, but discourage high-impact activities. Patients undergoing osteotomy frequently return to running and skiing after complete healing.
What’s the typical recovery time for each procedure?
Arthroscopy: 6-12 weeks for full recovery. Partial replacement: 3 months for most activities, 6 months for complete healing. Total replacement: 3 months for daily activities, 6-12 months for maximum improvement. Osteotomy: 6 months for return to activities, 12 months for complete bone healing.
Conclusion
Conservative treatments should be exhausted before considering surgery. When persistent knee pain limits daily activities or mechanical symptoms such as locking occur, surgical options provide targeted solutions tailored to your specific condition and lifestyle needs.
If you’re experiencing persistent knee pain, mechanical symptoms such as locking or catching, or knee instability that affects your daily activities, an orthopaedic surgeon can evaluate your condition and discuss appropriate treatment options.